Don't miss our updates


At Ingenes San Diego we understand how important this journey is for you. Our team combines cutting-edge technology with a close, personal approach to accompany you at every step, from the first evaluation to the most advanced reproductive techniques, always adapting to your needs. Who we are and what we offer We are a leading fertility clinic in assisted reproduction (ART). Here we perform in vitro fertilization (IVF), intracytoplasmic sperm injection (ICSI) and preimplantation genetic testing (PGT) in ISO-certified laboratories. We also offer egg vitrification, semen analysis and embryo culture with the highest quality standards. Our services: Comprehensive fertility evaluations (hormone panels, ultrasound) IVF/ICSI cycles with up to 1.5 mL of medium per embryo PGT for aneuploidy detection Egg and sperm cryopreservation Egg and sperm donation programs Counseling and emotional support throughout your process Your IVF process step by step 1. Ovarian stimulation and monitoring We personalize your protocol with daily injections (150–300 IU of follicle-stimulating hormone). We perform ultrasounds and estradiol measurements to track your follicle growth and choose the ideal time for egg retrieval. 2. Egg retrieval and fertilization Under light sedation, we use a 17-gauge needle to aspirate follicles in ≤10 mL of flushing medium. Eggs undergo IVF or ICSI depending on semen quality. 3. Embryo culture and transfer Embryos grow for 5–6 days in incubators with time-lapse imaging. We transfer one high-quality embryo to the uterus using a soft, ultrasound-guided catheter. Surplus embryos are vitrified at –196 °C. Why choose us? Our clinical pregnancy rates reach up to 55% per cycle in women under 35. We offer personalized counseling, financial plans and 24/7 support. Our certified reproductive endocrinologists design each protocol to maximize your safety and results, avoiding self-medication. We have geneticists, embryologists and mental health specialists to support you in every aspect of your path to parenthood. If you’re looking for nearby options, visit Ingenes Mexicali or discover Ingenes Fertility Specialists for home-based care. Key advantages Advanced genetic screening to reduce miscarriage risks Low-stress embryo transfers Comprehensive support: nutrition, psychology and finances CAP and CLIA accredited laboratory Frequently asked questions 1. How do I know if I need fertility treatment? If you’ve tried to conceive for more than 12 months (or 6 months if you’re over 35), consult a specialist. Irregular cycles, recurrent losses or conditions like PCOS and low ovarian reserve are signals to evaluate your fertility with hormone tests, ultrasounds and semen analysis. 2. What risks does IVF have and how do you manage them? IVF can cause ovarian hyperstimulation syndrome (OHSS), multiple pregnancies or procedural complications. At Ingenes we adjust doses, use “freeze-all” when necessary and transfer a single embryo to reduce risks. We have facilities and equipment ready for any eventuality. 3. Can I come if I live outside the U.S.? Yes. We assist with travel, visas and accommodation. We offer telemedicine and coordinate a comfortable stay in San Diego. If you prefer closer to Mexico, visit our sister clinic Ingenes Mexicali, with cultural and language support. 4. What emotional support do you offer? We have therapists specialized in reproductive health, support groups and individual sessions. We also offer mindfulness workshops and nutritional counseling so you don’t face this process alone. Sources American Society for Reproductive Medicine. Guidelines on Ovarian Stimulation. 2022. National Library of Medicine. In Vitro Fertilization. MedlinePlus. 2021. ESHRE Special Interest Group. Good Practice Recommendations for IVF Laboratories. Human Reproduction Open, 2020. Practice Committee ASRM. Criteria for Number of Embryos to Transfer. Fertility and Sterility, 2021. We’re with you every step of the way on this adventure. Don’t hesitate to seek accompaniment from an assisted reproduction specialist to resolve your doubts and care for your health.

“`html Each year, on June 4th, World Fertility Day is observed to raise awareness of the challenges millions of people face when trying to have a child and to promote real medical information, support, and solutions for those who wish to start a family. At Ingenes, this date is not just a symbolic celebration: it’s a moment to speak openly about a topic still burdened by stigma and misinformation. It’s an opportunity to remind everyone that there is hope, there are options, and that every story deserves respect, science, and empathy. What is world fertility day and why was it created? This day was established to break the silence around infertility and to remind us that fertility is a fundamental part of women’s and men’s health. The World Health Organization (WHO) recognizes infertility as a medical condition affecting at least 1 in 6 people worldwide. By observing this day, we aim to: Eliminate the stigma for those trying to conceive. Provide scientific, reliable information on causes and treatments. Reinforce that options exist, even in the most complex cases. At Ingenes, we join this global effort every June 4th with a message of hope and science. More details at Celebrating Hope and Science on World Fertility Day. How does infertility impact overall health? Fertility is linked to physical, hormonal, emotional, and social health. Infertility is not just a women’s issue; causes are distributed as follows: 40% female factors 40% male factors 20% mixed or unexplained A comprehensive diagnosis includes both partners (when applicable). Ingenes offers complete panels evaluating hormone levels, ovarian reserve (AMH in pg/mL), semen analysis (count in 106/mL), and imaging studies. Main causes of infertility in women and men In women Advanced age (over 35 years) Polycystic ovary syndrome (PCOS) Endometriosis Low ovarian reserve (AMH < 1.0 ng/mL) Blocked fallopian tubes Uterine abnormalities (fibroids, polyps, malformations) In men Low sperm count (oligozoospermia) Altered motility or morphology Hormonal imbalances (FSH, LH) Varicocele Infections or testicular injuries Other key factors: stress, BMI ≥ 25 kg/m2, smoking, excessive alcohol consumption, exposure to environmental toxins, and medical treatments like chemotherapy. Before taking any medication, consult a fertility specialist. When to see a fertility professional? Do not delay evaluation if any of these apply: Over 12 months of unprotected intercourse without pregnancy. Over 35 years old with no conception after 6 months of trying. Recurrent pregnancy loss. Known medical conditions affecting fertility. Single women or same-sex couples planning a baby. Previous treatments without results. Early diagnosis usually includes hormone profile, ultrasound, and semen analysis. Do not self-medicate: specialist guidance ensures a safe and effective path. Ingenes treatment options We offer a full range of assisted reproduction technologies, always personalized: Controlled ovarian stimulation Intrauterine insemination (IUI) In vitro fertilization (IVF) ICSI and PICSI Preimplantation genetic testing (PGT-A, PGT-M) Egg and sperm cryopreservation Egg or sperm donation Gestational surrogacy Advanced protocols like IVF MORE® for poor ovarian quality Each story is unique and each plan is crafted with scientific rigor and a human approach. More information at Celebrating World Fertility Day. Why is emotional support key? Infertility affects both mind and body. Anxiety, stress, and isolation can disrupt hormonal balance and treatment response. At Ingenes, we provide psychological counseling and support groups to care for both aspects: a healthy mind, a receptive body. Ingenes activities on World Fertility Day We share life and success stories. We offer webinars and educational materials. We reaffirm that fertility is a right for everyone. We remain committed: every attempt matters, every dream counts, and every baby born with Ingenes is the result of science, love, and perseverance. FAQs 1. What Lifestyle Changes Improve Fertility? A balanced diet rich in antioxidants, maintaining a BMI between 18.5 and 24.9 kg/m2, moderate exercise, and stress management with yoga or meditation benefit reproductive health. Avoid smoking, reduce alcohol, and limit exposure to endocrine disruptors. Get 7–8 hours of sleep and drink ≥ 2 L of water daily. Before taking supplements, consult a specialist to adjust folic acid, vitamin D, or CoQ10 doses. 2. Can Age-Related Infertility Be Reversed? Ovarian reserve declines with age, but treatments like ovarian stimulation and advanced IVF protocols (IVF MORE®) improve outcomes. PGT-A helps select chromosomally healthy embryos, increasing success rates. Egg donation is an option if reserve is very low. Emotional support and clear guidance are vital for confident decisions. 3. What’s the Difference Between Primary and Secondary Infertility? Primary infertility occurs when no pregnancy has ever been achieved after adequate attempts. Secondary infertility happens when difficulty conceiving arises after at least one previous pregnancy. Both require evaluation, though reproductive history and causes may affect the treatment plan. There is also unexplained infertility, when no cause is found. In such cases, assisted reproduction techniques are often the best alternative. 4. How Long Do Treatments Take Before Seeing Results? It depends on the protocol: IUI cycles last 2–3 weeks from stimulation to insemination; IVF cycles take 4–6 weeks (stimulation, egg retrieval, and transfer). Adding genetic testing adds a few more days. Emotional and physical preparation can add months. Each cycle provides valuable information to optimize the next. References World Health Organization. (2020). Infertility. https://www.who.int/news-room/fact-sheets/detail/infertility American Society for Reproductive Medicine. (2018). Definitions of Infertility and Recurrent Pregnancy Loss. Fertility and Sterility, 92(1), 1–2. MedlinePlus. (2021). Infertility. https://medlineplus.gov/infertility.html Klonoff-Cohen, H. (2005). Female and Male Lifestyle Factors and Fertility. We’re with you every step of the way. If you’re considering starting your family, don’t hesitate to seek the support of a fertility specialist: your story matters, and together we’ll find the best path to make it a reality. “`

Después de los 35 años, Cisne tuvo un embarazo con FIV y logró a sus 2 bebés, aún viviendo con ovario poliquístico. Ella te cuenta su historia.

Denisse te cuenta su historia, sobre su problema de infertilidad, y cómo después de un diagnóstico correcto logró tener a su primera bebita.

Las mujeres con ovario poliquístico pueden tener hijos. Claudia te cuenta cómo ella lo logró después de buscar a su bebé por más de 5 años.

Berenice tuvo abortos recurrentes debido a que vive con ovario poliquístico. Conoce su historia y cómo logró a su bebé en su 3er. ciclo de FIV.

Endometriosis is one of the leading conditions affecting women’s reproductive health and their ability to conceive. It often goes undiagnosed in time, which can complicate any assisted reproduction treatment. Although it is possible to become pregnant and have children with endometriosis, close monitoring by reproductive health specialists is essential to protect your well-being at every stage. Learn Blanca’s story and how she managed to have her baby despite this condition. What is endometriosis and how can it affect my chances of having a baby? Endometriosis occurs when tissue similar to the uterine lining grows outside the uterus, causing inflammation, scarring, and pain. This can alter fallopian tube function and ovarian reserve, reducing natural conception rates. Early diagnosis with transvaginal ultrasound or MRI and monitoring AMH (anti-Müllerian hormone) levels in ng/mL allow treatment personalization. Do not self-medicate: before taking any medication, consult an assisted reproduction specialist to increase your chances of pregnancy. What medical and surgical treatments are available for endometriosis? Options include hormonal suppression with GnRH analogs, progestogens, or combined oral contraceptives to reduce lesion activity. If there are painful or obstructive cysts, laparoscopic surgery is recommended to remove endometriomas and adhesions (1–3 cm nodules). Post-surgical recovery lasts 2 to 4 weeks, after which your specialist may propose ovulation induction or IVF. Can I get pregnant with IVF if I have endometriosis? Yes. Many women with endometriosis achieve pregnancy through personalized IVF, optimizing ovarian stimulation, oocyte retrieval (8–15 follicles of 2–20 mm), and embryo transfer. Success rates depend on age, ovarian reserve, and lesion severity, but specialized care at centers like Ingenes significantly improves outcomes. How to choose the right specialist for endometriosis? Look for a reproductive endocrinologist experienced in endometriosis, with access to advanced imaging and a proven track record in assisted reproduction. Read reviews and testimonials—such as “I became a mom despite having endometriosis”—to learn about care quality and patient support. A multidisciplinary team offers comprehensive care. What lifestyle changes help fertility with endometriosis? A balanced diet rich in omega-3 fatty acids and antioxidants, avoiding inflammatory foods (gluten, dairy), is key. Engage in gentle exercise, practice stress management techniques (yoga, mindfulness), and get good sleep to maintain hormonal balance. Quit smoking and limit caffeine to under 200 mg/day (≈2 cups of coffee). Blanca’s success story with endometriosis and IVF “At 35, I was diagnosed with endometriosis and told I had a 0% chance of becoming a mother. After several misdiagnoses and a very painful hysterosalpingogram, I lost hope. In 2018 a friend recommended Ingenes: there they told me I had PCOS and endometriosis, but that I could succeed. Their IVF protocol gave me a positive result on the first attempt.” “I didn’t discover my pregnancy until the fourth month, when I found out I was having a girl. Holding María Eugenia in my arms changed my life: she is perfect. The journey was difficult, but Ingenes’ expert care and personalized treatment gave me my greatest joy.” How to start your path to pregnancy with endometriosis? If you also have endometriosis or another fertility challenge, schedule a consultation with a specialist. At Ingenes we offer an Initial Program to evaluate your medical history, hormonal profile, and previous cycles, and design a plan tailored to you. This is the path that will bring you closer to your little star. FAQ 1. Can endometriosis go away on its own? It is a chronic condition that does not resolve without intervention. Hormonal treatments suppress symptoms, but surgical removal is often necessary to eliminate the tissue. After surgery, medical therapy reduces the risk of recurrence. Regular follow-up with imaging and clinical evaluation ensures early detection of new lesions. Lifestyle adjustments and specialist support maintain quality of life and reproductive potential. 2. What risks come with delaying fertility treatment for endometriosis? Delaying treatment can cause lesions to grow, more scarring, and diminished ovarian reserve. In advanced stages (III–IV), natural conception rates drop and the IVF protocol becomes more complex. Timely intervention helps preserve ovarian function, improves assisted reproduction success rates, and relieves chronic pain. Consultation within six months of diagnosis is recommended. 3. How does endometriosis affect IVF success? It can reduce ovarian response, fertilization, and increase miscarriage risk. However, with personalized gonadotropin dosing, surgical management of endometriomas, and embryo vitrification, rates comparable to other indications are achieved. Centers experienced in endometriosis, like Ingenes, report live birth rates over 40% per cycle in patients under 38 years old. 4. Are there non-hormonal therapies for endometriosis pain? Yes. NSAIDs (ibuprofen 400 mg every 6–8 hours) relieve pain. Complementary therapies—acupuncture, pelvic physiotherapy, and dietary changes—can reduce inflammation and pain perception. Always consult your specialist before integrating adjunct therapies so they align with your fertility goals. Sources National Library of Medicine. (2023). Endometriosis. MedlinePlus. https://medlineplus.gov/endometriosis.html Giudice, L. C. (2010). Clinical practice. Endometriosis. The New England Journal of Medicine, 362(25), 2389–2398. doi:10.1056/NEJMcp1000274 Practice Committee of the American Society for Reproductive Medicine. (2012). Endometriosis and infertility: a committee opinion. Fertility and Sterility, 98(3), 591–598. doi:10.1016/j.fertnstert.2012.05.019 Santulli, P., & Borghese, B. (2016). Endometriosis: epidemiology, classification, pathogenesis, treatment and genetics. International Journal of Molecular Sciences, 17(5), 777. doi:10.3390/ijms17050777 Remember that every story is unique: you are not alone. Consult a reproduction specialist for personalized guidance and support on your journey to parenthood.

Guadalupe utilizó el método ROPA para quedar embarazada y ser madre de Matías junto a su esposa. Un bebé de ambas, conoce su historia aquí.

¿Se puede quedar embarazada con quistes en los ovarios? Conoce a Rosy, una mujer de más de 35 invadida de quistes, y cómo logró a su bebé.

A los 36 años, Conny tuvo problemas para ser mamá de nuevo. Su esposo tenía la vasectomía, pero pudieron lograrlo con una fecundación in vitro.

At Ingenes, we are excited to announce that we will host two scientists from Oregon Health & Science University (OHSU), world leaders in gene therapy and reproductive biotechnology. Together, we will advance the IVF MORE® (Magnetic Ovulatory Restoration) technique, an innovative approach designed to improve your egg quality and increase your chances of success in assisted reproduction. What is IVF MORE® and how does it help you? IVF MORE® combines nuclear transfer and mitochondrial replacement so your eggs regain energy and quality. We use 2 mL of optimized cell solutions and 0.5 mL of enriched media to restore mitochondrial function in eggs with low reserve. It is especially indicated if you have had unsuccessful IVF cycles or low oocyte quality. With IVF MORE® we increase the viable embryo rate and improve implantation. OHSU – Ingenes collaboration During the visit of Doctors Shoukhrat Mitalipov and Nuria Martí-Gutiérrez, we will hold a Scientific Exchange on IVF MORE®. We will share ovarian restoration and stem cell reprogramming protocols. With this alliance, we reaffirm our leadership in Latin America in nuclear transfer and gene therapy for assisted reproduction. If you want to increase your pregnancy options, consult an Assisted Reproduction specialist first. First Ovarian Restoration Session In the initial session, we apply follicular biopsy and mitochondrial reconstitution to rejuvenate your eggs. We extract somatic cells to obtain healthy mitochondria and incorporate them into the eggs via microinjection under a stereoscopic microscope. This exclusive protocol offers an alternative to egg donation. Each plan is personalized after detailed serum hormone (KG) and AMH diagnostics. Avoid self-medication: trust your specialist. The key role of our laboratory Our laboratory features controlled-atmosphere incubators, time-lapse systems for embryo monitoring, and state-of-the-art sequencers. This way, we optimize every phase of IVF. Here we perform preimplantation genetic testing (PGT) to ensure you transfer only top-quality embryos. Learn more about the vital role of the laboratory in our IVF process. 20 years of fertility innovation In 2025, we celebrate 20 years of transforming lives with a multidisciplinary team and cutting-edge technology. If you’re ready to take the next step toward parenthood, IVF MORE® could be the answer you’ve been looking for. Contact our specialists and discover your personalized path. Frequently Asked Questions Who are the OHSU specialists and what do they bring? Doctors Mitalipov and Martí-Gutiérrez are leaders in nuclear transfer and mitochondrial replacement. They bring advanced protocols to restore ovarian function for those with poor egg quality. How does IVF MORE® differ from conventional IVF? IVF MORE® adds healthy mitochondria and cellular reprogramming to enhance oocyte viability. This translates into higher embryo cleavage rates and better implantation, especially after failed cycles. At what age is it recommended? It is especially recommended for women with low ovarian reserve or over 38 years old. Each case is evaluated with hormonal tests (FSH, AMH) and ultrasound, and the appropriate hormone dosage is designed. What precautions should I take? Do not self-medicate. Have a complete hormonal profile done and share your history with your specialist. Maintaining a balanced diet, moderate exercise, and stress management improves your ovarian response. Sources Consulted National Library of Medicine (2022). Mitochondrial Replacement Therapy. https://medlineplus.gov/mitochondrialreplacementtherapy Harvard T.H. Chan School of Public Health (2021). Assisted Reproductive Technologies. https://doi.org/10.1002/9781119156805 ESHRE (2020). Guidelines on IVF. https://www.eshre.eu/Guidelines-and-Legal/Guidelines/IVF ASRM (2019). Nuclear Transfer in Human Embryos. Fertility and Sterility, 112(6), 1009-1020. https://doi.org/10.1016/j.fertnstert.2019.08.015 We know this journey can be challenging. You’re not alone! Consult an in vitro fertilization specialist for personalized guidance and support.

Ana tuvo problemas de tiroides, quistes y con sus trompas de Falopio, conoce su testimonio de fecundación in vitro y cómo logró tener a sus cuatitos.

Baja reserva ovárica y FIV positiva en su tercer intento, conoce a Claudia, quien se convirtió en mamá después de varios tratamientos fallidos.
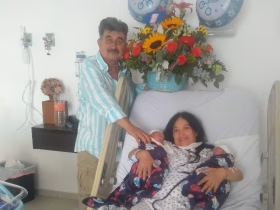
Conoce la historia de María del Carmen y cómo logró su embarazo con ligadura de trompas, aún teniendo 50 años y su esposo 58.

Fernanda tuvo su embarazo con ovario poliquístico, al realizar un tratamiento multiciclo de Fertilización In Vitro, aquí te cuenta su historia.

Cecilia se convirtió en mamá de Angélica al tener un embarazo a los 48 años. Conócela aquí y sobre el tratamiento FIV que lo hizo posible.

Soy Claudia, tengo endometriosis y quedé embarazada. Conoce su historia y cómo vive este padecimiento que afecta a 7 millones de mexicanas.

Female fertility declines with age, and achieving pregnancy naturally after 35 is usually more challenging and carries higher risks. Thanks to advances in assisted reproduction, today it’s possible to become a mom or dad with fewer obstacles, even after 40, through fertility treatments. Learn Olga’s story, who at 43 fulfilled her dream of becoming a mother thanks to a multicycle In Vitro Fertilization program. What complications arise when trying to conceive at 43? Olga – Ingenes mom “We went through painful procedures without finding the cause: ‘infertility of unknown origin.’ My husband and I thought it was almost impossible to make it in time. Over the years I understood that, even though we postponed motherhood, that hope remained alive.” How does the biological clock impact you after 40? Angelique – Olga’s daughter “I was 43 and my husband was 47; since it was my first pregnancy everything got complicated. We tried to conceive without help, but after 1.5 years and two clinics with no success, the emotional toll was immense: tests, ultrasounds, hysterosalpingograms…” What role does social pressure play? The pressure is intense. Even if you don’t believe “a woman only fulfills herself by being a mother,” when you want it with all your heart, every setback hurts and affects your mood, self-esteem and creates anxiety. Angelique celebrating with her parents and grandmother I almost gave up and thought about adoption. My husband and I supported each other and decided to give it one last try. It was the best decision of our lives. How did Olga succeed with IVF at Ingenes? I arrived at Ingenes in 2015 and, after three years of persistence, the final IVF cycle was intense: daily labs, follicle monitoring, egg retrieval and embryo transfer. Three months later, seeing the heartbeat on the first ultrasound made it all worthwhile. When the doctor said, “it’s a girl,” our hearts exploded with emotion. Angelique’s first cry at birth was the most sublime moment: pure joy and relief. Angelique in her ball pit Angelique brightened our lives and taught me that at 43, motherhood transforms everything: priorities, passions and the meaning of being. Options for women over 40 Becoming a mother at 40 is possible. At Ingenes we design a personalized plan that optimizes your chances in the shortest time. With our Initial Program we thoroughly evaluate your fertility. Our Assisted Reproduction specialists guide you every step of the way. Share your story or read testimonials: single mom at 43 or mother at 40. Soon you’ll be holding your baby. Frequently Asked Questions What is the success rate of IVF in women over 40? The IVF success rate between ages 40 and 45 ranges from 10% to 30% per cycle, depending on ovarian reserve and embryo quality (Human Reproduction; Fertility and Sterility). Preimplantation genetic testing (PGT-A) increases the chance of clinical pregnancy. What risks come with pregnancy at 43? The risk of hypertension, gestational diabetes and premature birth is up to double compared to women under 35 (Mayo Clinic; MedlinePlus). Strict obstetric monitoring, regular ultrasounds and surveillance of glucose and blood pressure reduce complications. How do stress and emotional support influence outcomes? Chronic stress alters the hypothalamic-pituitary axis, affecting ovulation and implantation (Journal of Assisted Reproduction and Genetics). Psychological support and support groups improve success rates. Is self-medicating with fertility treatments advisable? Do not self-medicate. The dosage and combination of drugs for ovarian stimulation require medical supervision. A specialist will design your protocol based on your hormonal profile and history, with monitoring via ultrasounds and lab tests. Sources American Society for Reproductive Medicine. Evaluation and Treatment of Infertility: A Guide for Patients (2020). MedlinePlus. In Vitro Fertilization (2022). Practice Committee ASRM. Testing and interpreting measures of ovarian reserve (Fertility and Sterility, 2017). Mayo Clinic. Pregnancy after 40: Health risks for mother and baby (2021). We know how challenging this journey can be. You are not alone: trust in your strength and seek professional support. Consulting a fertility specialist can make the difference in your life story.

Getting pregnant at 40 is possible and safe. After 35, the quality and quantity of eggs decrease, reducing the chances of conceiving. It’s a natural process, but Assisted Reproduction Technologies (ART) help you “stop the biological clock” and achieve a baby even after 40. Below, Ruth shares how at 44, with a multicycle In Vitro Fertilization treatment, she fulfilled her dream of becoming a mother. What challenges does getting pregnant at 40 pose? “I had ruled out motherhood; I thought it was no longer possible because of my age. When I met my husband, trying again became a big dream.” At 44, after six months of natural attempts, Ruth went to Ingenes. Although she ovulated regularly and had no uterine issues, conception didn’t happen. Tailoring IVF for women over 40 In her first cycle, the emotional ups and downs were intense. “My doctor and nurse gave me patience and warmth. Feeling secure made all the difference.” After a failed attempt, they discovered a cervical constriction via hysteroscopy and designed a custom protocol for her. The success of the second transfer With the second transfer, Benjamin was born. “I rested for a month to recover, returned from Las Vegas to Mexico, and received the greatest blessing.” When she heard him cry, she felt her soul return. “Today my heart beats outside of me through my child.” Key treatments and support after 35 If you are over 35 and haven’t conceived after 6 months, see a specialist. ART includes ovarian stimulation, ICSI, egg donation, and preimplantation genetic diagnosis. At Ingenes, our Initial Program offers: Hormone profile and AMH levels (ng/mL). Antral follicle count by ultrasound. Personalized treatment plan. If you want to share your story, tell us here. You can also read other testimonials like “Pregnancy at 48 with low ovarian reserve” and “Mother at 40”. FAQ about pregnancy at 40 Is pregnancy after 40 risky? There may be a higher risk of hypertension and gestational diabetes, but with check-ups every 4–6 weeks and a BMI between 18.5–24.9, these risks decrease. A balanced diet with 0.8 g/kg of protein daily helps maintain health. Specialists also recommend folic acid (400 µg daily) and 30 mg of iron per day, all under medical supervision. How long should you try naturally before seeing a specialist? Under 35: consult after 12 months without results. Over 35: ideally at 6 months. Early diagnosis with FSH, LH, AMH tests, and antral follicle ultrasound optimizes your treatment. What is an antral follicle count? It measures the small follicles in the ovaries by ultrasound. Between 8 and 12 follicles indicate good reserve; fewer than 5 may suggest low reserve and recommend egg donation. Along with AMH, it helps adjust the FSH dose (up to 375 IU daily). How does egg quality affect late conception? With age, chromosomal aneuploidy increases and the rate of euploid embryos drops to 10% between 40 and 45 years. That’s why PGT-A is useful to select healthy embryos. Combined with multi-egg cycles, success can reach 50% per transfer. Sources consulted American Society for Reproductive Medicine. Age and fertility: a guide for patients. 2020. National Institutes of Health. Fertility (male and female). 2022. Practice Committee ASRM. Testing and interpreting ovarian reserve. Fertility and Sterility. 2015. World Health Organization. WHO recommendations on preconception. 2018. We know this journey can be challenging. You are not alone: seek the support of an assisted reproduction specialist to receive the right guidance and treatment. Your dream of becoming a mother or father is closer than you think.

Motherhood is a right for everyone, regardless of economic status, nationality, race, or age. Deciding to have a child is one of life’s most beautiful experiences, and each person chooses the moment they feel is ideal. It’s true that as the years go by the chances of pregnancy decrease, but they don’t disappear. Many women achieve their dream at stages they thought were impossible. Assisted Reproduction Technology has transformed the lives of those who want to become mothers. A clear example is Carolina, who in her forties welcomed her daughter Cielo. How did I become a mom after 40 thanks to assisted reproduction? “On May 10, 2018, I discovered I was pregnant. The doctor confirmed it and my husband sent me a photo with baby socks: we were going to be parents!” – Carolina Carolina and Fernando celebrate the arrival of their daughter Cielo “I cried with emotion: it was the most beautiful news of my life. Now my goal is to enjoy every moment with her, while life allows us.” – Carolina Challenges during my pregnancy at 40 My pregnancy was smooth, although I developed gestational diabetes, which I managed with a balanced diet and gentle exercise. My husband supported me in everything, sweetening my cravings with fresh fruit and low-carb desserts. Cielo dressed as a pumpkin on her first Halloween My journey to conception with In Vitro fertilization After five years of trying and three unsuccessful intrauterine inseminations, we started our first in vitro fertilization cycle. It didn’t work, but the medical team encouraged us to continue. In the next cycle, my husband and I took hormonal medication: 150 IU daily of subcutaneous FSH and 0.25 mg of a GnRH antagonist, according to a personalized ovarian stimulation protocol. Fernando holds his little daughter Cielo The most exciting moment When they brought out Cielo and I saw her for the first time, I cried with joy. She weighed 3.2 kg and measured 51 cm, with beautiful hair. My husband and our doctors were by my side: my heart exploded with love. Cielo’s first birthday, surrounded by love Inspiration to become a mother after 40 Cielo is my greatest gift. Thanks to her, I learned to value every moment and always show her the light of life. Every kiss from her fills me with energy and hope. Carolina and Cielo at her baptism, an unforgettable day Options to get pregnant at 40 With age, ovarian reserve and egg quality decrease, and risks like miscarriage or complications such as diabetes or hypertension increase. But the good news is that assisted reproduction offers: Egg or sperm donation Gamet cryopreservation Personalized stimulation protocols At Ingenes Institute we have been changing lives for 17 years with our IVF lab, egg bank, sperm bank, and a team of committed specialists. Read more stories: Single mom at 40: my brave decision Single mom at 46: my dream fulfilled FAQ – Frequently Asked Questions 1. Is it safe to get pregnant after 40? There is a higher risk of complications such as gestational diabetes, hypertension, or miscarriage. With medical follow-up, a balanced diet, and moderate exercise, many women have healthy pregnancies. Never self-medicate: always consult a specialist. Assisted reproduction evaluates your ovarian reserve with AMH tests and antral follicle count (AFC) to design a stimulation plan that maximizes your chances. 2. What assisted reproduction treatments are recommended for women over 40? The most effective are in vitro fertilization (IVF) with or without ICSI and, when ovarian reserve is low, egg donation. A specialist in assisted reproduction will guide you to the best option. Egg donation has over a 50% pregnancy rate per cycle with young eggs. Plus, vitrification allows you to preserve your fertility for the future. 3. How do diet and lifestyle influence fertility at 40? A diet rich in antioxidants (fruits, vegetables, oily fish) and low in ultra-processed foods improves egg quality. Maintaining a healthy BMI (18.5–24.9 kg/m²), avoiding alcohol and tobacco, and reducing stress with yoga or meditation boosts your fertility. Supplements like folic acid (400 µg/day), vitamin D (1,000–2,000 IU/day), and Coenzyme Q10 (100 mg/day) support mitochondrial function in eggs and reduce oxidative stress. 4. What should I know before choosing an egg or sperm bank? Check the laboratory’s certification, sample quality (morphology, motility), and donors’ genetic testing. A good bank offers genetic and psychological counseling for an ethical, transparent process. Ask about post-thaw survival rates, infectious and genetic screenings performed, and the total cost. Always look for international standards. Sources Consulted Office on Women’s Health. (2022). Fertility and Age. https://www.womenshealth.gov Practice Committee ASRM. (2015). Testing and interpreting measures of ovarian reserve. Fertility and Sterility, 103(3), e9–e17. MedlinePlus. (2023). Gestational Diabetes. https://medlineplus.gov/spanish/diabetesgestacional.html ACOG. (2021). Advanced maternal age. Obstetrics & Gynecology, 138(3), e7–e9. You’re taking an important step toward your dream. Rely on a specialist in assisted fertilization: you and your future baby deserve the best care!

Una mala calidad de óvulos no impide que tengas un bebé. Iraí te comparte su camino y el tratamiento específico que la ayudó a lograrlo.

Rebeca pasó por un diagnóstico de ovario poliquístico, endometriosis y una cirugía innecesaria, antes de lograr a sus bebés in vitro. Conoce su historia aquí.

An incorrect fertility diagnosis can delay the dream of becoming a mom or dad and lead to treatments that don’t match what the patient really needs, especially when uterine fibroids are involved. This is how Denisse and her husband lived for 8 years: after several attempts they decided to turn to Ingenes for a comprehensive fertility diagnosis. Discover their story. What challenges do uterine fibroids pose for conceiving? Denisse, Ingenes mom “I had been trying to have a baby for 8 years. My husband and I left Venezuela for Querétaro, Mexico. We did three cycles of artificial insemination and two IVF attempts, but we always ended up disappointed. I felt alone and overwhelmed; I didn’t understand why fibroids—benign growths in the uterus—were overshadowing our dream. When a fibroid distorts the cavity, it can hinder implantation or cause recurrent miscarriages. How did the IVF experience change when moving to Mexico City? When we arrived in Mexico City we met the Ingenes team. In the first consultation I asked for total clarity: “Tell me what’s happening and if I can become a mother.” The diagnosis was uterine fibroids and, although I was frightened at first, the doctor explained that IVF was still an option. That certainty gave us hope again. Ingenes family enjoying an outing What emotions arise when undergoing IVF with fibroids? “The day they told me I was pregnant, my heart was racing a thousand miles an hour. My husband and I cried with joy. But at 8 weeks I had bleeding that filled me with fear and sleepless nights, thinking our dream was slipping away. The next day, when I heard the baby’s heartbeat—‘thump, thump, thump’—on the ultrasound, I knew our daughter was strong. That sound turned my anxiety into certainty that we could overcome any obstacle. Why is a personalized treatment vital when fibroids are present? Becoming a mother through assisted reproduction is possible! Fibroids vary in size (cm) and location; that’s why each plan must be tailored: from surgery to specific IVF protocols. Avoid self-medicating and before taking any medication, talk to a reproductive medicine specialist. At Ingenes we offer our Initial Program, a comprehensive evaluation with a hormonal panel (FSH, LH, AMH) and imaging studies (ultrasound with measurements in mm) to discover what is preventing your pregnancy. Our assisted reproduction specialists design the ideal plan, which may include laparoscopic myomectomy or adjusted stimulation protocols to improve your chances. Read similar cases, such as “After 10 years trying and with fibroids, I had my baby” or “I became a mom despite having endometriosis” and find out how others overcame their challenges. Frequently Asked Questions 1. Can fibroids reduce IVF success? Yes. Submucosal fibroids, which invade the uterine cavity, distort the endometrium and lower implantation rates. Studies indicate that hysteroscopic myomectomy can raise IVF success from ~30% to over 40% per cycle. Intramural or subserosal fibroids (measured in cm) tend to affect less, depending on size and number. A personalized imaging evaluation determines if surgery is necessary before IVF. 2. What fibroid size requires removal before IVF? Generally, fibroids ≥3 cm compressing the cavity should be removed to improve implantation. Those under 2 cm outside the uterus can be monitored. The decision depends on symptoms (bleeding, pain) and reproductive plans. Always consult your specialist to weigh risks and benefits. 3. How long to wait after myomectomy before starting IVF? Recovery time varies: laparoscopic surgery requires 6–8 weeks, open surgery up to 12 weeks for uterine healing. Do not attempt pregnancy until the doctor confirms uterine integrity with an ultrasound. Once approved, optimal ovarian stimulation is planned and embryo transfer is scheduled under the best conditions. 4. Are there non-surgical alternatives to treat fibroids during fertility? Yes. GnRH agonists can reduce fibroids (mL or mm) by inducing a temporary hypoestrogenic state. Treatment lasts 3–6 months and can decrease fibroid volume by up to 50%. Uterine artery embolization is another option, though its impact on ovarian reserve (AMH in ng/mL) must be carefully evaluated. Talk to your reproductive endocrinologist to choose the best strategy. References ACOG. (2021). Uterine Fibroids: ACOG Practice Bulletin No. 228. Obstetrics & Gynecology, 137(6), e100–e115. https://doi.org/10.1097/AOG.0000000000004656 National Library of Medicine. (2022). Fibroids and Infertility. MedlinePlus. https://medlineplus.gov/fibroidsandinfertility.html Practice Committee of the American Society for Reproductive Medicine. (2020). Role of fibroids in infertility. Fertility and Sterility, 114(3), 477–488. https://doi.org/10.1016/j.fertnstert.2020.05.030 Stewart, E. A. (2019). Uterine fibroids. The New England Journal of Medicine, 380(14), 1314–1325. https://doi.org/10.1056/NEJMra1801438 We know how challenging this journey can be. Don’t lose hope or self-medicate: always consult a fertility specialist to guide you every step of the way.
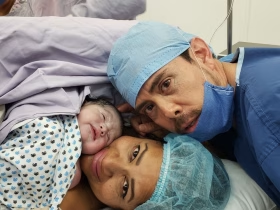
Tener un bebé por medio de una ovodonación no es una decisión sencilla y, por eso mismo, requiere que cuentes con información precisa, y que tomes un tiempo para analizar esto junto con tus deseos de maternidad. Es por eso que te compartimos la historia de Lorena, quien debido a su baja reserva ovárica, recurrió a la donación de óvulos para tener a su pequeña mediante una FIV.

When you try to conceive a baby, the journey can be challenging and full of emotional and physical ups and downs. If you suffer from adenomyosis or another infertility condition, you know that doubts and fear can grow. Eridani’s story shows that there is hope. She overcame adversity thanks to Assisted Reproduction Methods and today enjoys the joy of being a mom. Eridani, proud Ingenes mom What is adenomyosis and how does it affect fertility? Adenomyosis occurs when the tissue that normally lines the uterus grows into its muscular wall. This often causes heavy bleeding (up to 200 ml per cycle), pelvic pain, and an enlarged uterus (sometimes 1–2 kg heavier). All of this can make embryo implantation difficult and reduce natural fertility. Some women have severe cramps, others mild discomfort. It is usually diagnosed between ages 40 and 50, but it also affects women in their 30s and even late 20s. It is detected with a transvaginal ultrasound or MRI. Treatments range from hormonal therapy to minimally invasive surgery, always tailored to your motherhood goals. Do not self-medicate: always consult a specialist. How did Eridani overcome adenomyosis to conceive? “I told Enrique, ‘If you want, find someone else, I’m the problem.’ It was very hard. My life was just work until I got married and discovered my longing to become a mom.” After almost 3 years of trying in Mexico and New York with no results, she came to Ingenes. There they confirmed endometriosis, adenomyosis, and poor egg quality. With a personalized ovarian stimulation protocol (225 IU of FSH daily) and careful embryo culture, she achieved a successful twin pregnancy. Ingenes babies feeding Assisted reproduction options for adenomyosis It depends on your age, the severity of adenomyosis, and your motherhood plans. Options include: Hormonal suppression (GnRH agonists) to reduce the uterus by up to 30% in 3–6 months. Minimally invasive surgery (adenomyomectomy) to remove lesions and preserve the uterus. In vitro fertilization (IVF) with stimulation and frozen embryo transfer. Before any medication or procedure, consult a specialist in Assisted Reproduction. Emotional and practical tips during treatment Keeping stress under control and a healthy lifestyle helps a lot. Try: Yoga or mindfulness to reduce cortisol. A diet rich in omega-3 and antioxidants. Support groups or therapy to share experiences. With your partner’s love and your trusted network, the process will be more bearable. Proud Ingenes parents with their daughters For more inspiring testimonials, visit: I became a mom despite having endometriosis and I had uterine fibroids and became a mother with IVF. How to start your journey to motherhood with adenomyosis? Schedule an evaluation with a fertility specialist. They will review your history, perform imaging studies, and propose a personalized plan. Early detection and timely treatment can make all the difference. Frequently Asked Questions 1. Can adenomyosis go away on its own? No. Without intervention it usually worsens, with more bleeding and pain. Early diagnosis allows for medical management that improves your quality of life. 2. Does it affect pregnancy outcomes? It increases the risks of miscarriage, preterm birth, and placental complications. With personalized protocols, such as GnRH pre-treatment before IVF, success rates improve. 3. Natural remedies for pain? Thermotherapy, anti-inflammatory diets, and supplements (omega-3, turmeric) can help, but never replace medical treatment. Always consult your doctor. 4. Adenomyosis vs. endometriosis? Both involve endometrial tissue outside its normal location. In endometriosis it is on pelvic organs and the peritoneum; in adenomyosis, it is within the uterine muscle. Management differs, so good imaging is key. Sources consulted American College of Obstetricians and Gynecologists. Practice Bulletin No. 228: Management of Endometriosis. Obstetrics & Gynecology, 135(4), e65–e81. doi:10.1097/AOG.0000000000003774 National Library of Medicine. (2021). Adenomyosis. MedlinePlus. https://medlineplus.gov/adenomyosis.html Harmsen, M. J. A., et al. (2019). Adenomyosis: Prevalence, risk factors and therapeutic options. Best Practice & Research Clinical Obstetrics & Gynaecology, 65, 40–49. doi:10.1016/j.bpobgyn.2019.01.002 Vercellini, P., et al. (2017). Medical treatment for adenomyosis: A systematic review. International Journal of Obstetrics & Gynaecology, 124(1), 3–8. doi:10.1111/1471-0528.14301 We are with you every step of the way. Remember that seeking professional help in assisted reproduction could be the key to making your dream of becoming a mother or father come true.

When the desire to have a child is so strong, nothing and no one can stop it. Assisted reproduction breaks down barriers, pushes science to the limit to create life, and connects with the deepest longing of many couples. How much do you dream of becoming a mother or father? Here is Luz’s story, who had to choose between staying in her marriage or pursuing her dream of starting a family. What is skin-to-skin contact and why is it so powerful? “When Leonardo was born and they placed him on my chest, I couldn’t believe it: he finally existed! He stayed skin-to-skin with me for an hour… in that moment everything is forgotten, it’s an indescribable love.” Skin-to-skin contact right after birth stabilizes the baby’s temperature and heart rate, strengthens the bond, and triggers the mother’s oxytocin, creating a deep emotional connection. Luz and her husband traveled a long road to reach that moment. She was 33 when she said, “I thought I could give up that part of my life, but no: I want a baby, and if you don’t, we should separate.” That decision marked the beginning of her assisted reproduction journey. What factors led Luz to assisted reproduction? After trying naturally, Luz was diagnosed with polycystic ovary syndrome (PCOS) and her husband with teratozoospermia, conditions that lowered their chances of conceiving to 10%. They then decided on in vitro fertilization (IVF): in a laboratory, eggs and sperm are combined, and healthy embryos are transferred to the uterus. Thanks to advances in reproductive medicine and a personalized protocol with ovarian stimulation of 225 IU of gonadotropins, Luz achieved a twin pregnancy on the first cycle. Leonardo and Daniela were born healthy after careful monitoring and neonatal care. How did IVF change Luz’s life and what can you expect? “It wasn’t easy, but when you’re in treatment you realize how many people can’t become parents—it’s more common than you think, and that helps… we were lucky: it worked on the first try. Twins: Leonardo and Daniela. They took a while to hand me Daniela because they wanted to check her, but then she was perfect.” IVF success rates vary by age and clinic; for women under 35, they hover around 40% live births per cycle. At INGENES, embryologists use time-lapse incubators and preimplantation genetic testing (PGT-A) to select the strongest embryos and increase implantation chances. Can assisted reproduction make your dream of becoming a parent come true? The technology available today in Mexico at institutions like INGENES provides solutions for those who have not yet conceived: IVF, ICSI, egg vitrification, and donation programs, with protocols tailored to your needs. If you entrust us with your story, together we will write the best chapter. We know some paths are long, but at INGENES we turn them into an adventure with a clear direction: your family. Discover our assisted reproduction treatments and take the first step toward your baby. Frequently Asked Questions 1. What is in vitro fertilization and how does it work? IVF is an assisted reproduction procedure in which eggs are retrieved from the ovaries, fertilized with sperm in a laboratory, and after several days of culture, a viable embryo is transferred to the uterus. During ovarian stimulation, 150–300 IU of gonadotropins are administered to develop multiple follicles. IVF success depends on age, gamete quality, and laboratory expertise. In women under 35, implantation rates can reach 40% per cycle. Before starting, consult a reproductive medicine specialist to assess your case. 2. What risks and care are involved after an IVF cycle? Risks include mild ovarian hyperstimulation syndrome, which can cause abdominal bloating and general discomfort but is controlled by adjusting medication. There is also a low risk of multiple pregnancies; that’s why at INGENES we recommend transferring a single embryo whenever possible. After transfer, rest moderately for 24 hours, maintain a calm routine, and avoid strenuous physical activity. Do not self-medicate without consulting. Progesterone supplementation (e.g., 600 mg/24 h vaginally) supports implantation and reduces miscarriage risk. 3. How do emotional support and the partner influence treatment success? Psychological support reduces stress and anxiety, improves hormonal balance, and endometrial receptivity. Studies show patients with emotional support have a 10–15% higher chance of achieving pregnancy. Involving the partner at every stage, from stimulation to control ultrasounds, strengthens the bond and shares the emotional load. At INGENES we offer counseling sessions for couples and personalized nutritional advice. 4. What alternatives are there if the first IVF cycle doesn’t work? If pregnancy is not achieved, factors such as embryo quality, endometrial receptivity, and genetics are reviewed. Additional tests like PGT-A can be incorporated or the protocol adjusted. Egg or sperm donation and surrogacy are options in cases of repeated failure or uterine factor. Before deciding, review your results with the specialist to define the most appropriate path. Sources American Society for Reproductive Medicine. (2021). In vitro fertilization (IVF). Retrieved from https://www.asrm.org MedlinePlus. (2022). Assisted reproductive technology. Retrieved from https://medlineplus.gov/assistedreproductivetechnology.html Kassabji, M., & Holmes, M. (2020). The impact of psychological support on IVF outcomes: A systematic review. Human Reproduction Update, 26(3), 350–364. doi:10.1093/humupd/dmz043 Practice Committee of the American Society for Reproductive Medicine. (2019). Diagnostic evaluation of the infertile female: A committee opinion. Fertility and Sterility, 111(1), 9–13. doi:10.1016/j.fertnstert.2018.11.034 We know how important your longing to become a parent is. If you have questions, seek the support of an assisted reproduction specialist to receive the guidance and care you and your partner need.

Becoming a mother is a decision filled with emotion and meaning. Lluvia decided to do it on her own at 40, embarking on a journey of courage and hope. Nowadays, more women choose to become mothers without a partner, either by conviction or life circumstances. Through Lluvia’s story you’ll learn about her motivations, the challenges she faced, and her experience as a single mother thanks to assisted reproduction. Discover how science opened doors for her and read real testimonials like “I Became a Mother at 40” and “I Wanted to Be a Single Mother and Finally Had My Babies at 46.” What motivates a woman to become a single mother at 40? Lluvia always felt a very strong maternal instinct. Upon turning 40, concerns about her biological clock and social expectations led her to decide: use her own eggs and a trusted friend as sperm donor. Avoid self-medication and seek professional guidance to assess your ovarian reserve with tests like AMH and antral follicle count. Before starting, consult a specialist in Assisted Reproduction to design a personalized plan. What challenges does single motherhood with IVF at 40 entail? Age reduces egg quality and quantity. After detecting a fibroid, Lluvia underwent myomectomy and waited eight months before IVF. She faced emotional stress, uncertainty, and the routine of daily FSH and LH injections (around 225 IU). Physical recovery and anxiety over success rates (below 30% for women over 40) test one’s strength. Having a team of a reproductive specialist, psychologist, and nutritionist makes a difference in outcomes and well-being. How to prepare for fertility treatments at 40 as a single woman? A diet rich in folates and antioxidants, 50 g of protein daily, avoiding tobacco and excess caffeine, and taking 400 µg of folic acid are good first steps. Moderate exercise, yoga, and mindfulness help hormonal balance. Have ovarian reserve tests, pelvic ultrasound, and infection screening done as soon as possible. Support from counselors or online groups reduces loneliness and maintains motivation. What support exists for single mothers undergoing IVF? Specialized clinics offer financial counseling, legal support for donation agreements, and psychological assistance. Online communities connect women with similar experiences, reducing isolation. Scholarship programs or shared risk plans lower costs, and the testimony of other mothers—like “I Became a Mother at 40”—provides practical advice and hope. Emotional journey after IVF success After a positive pregnancy test, many maintain cautious optimism. Lluvia waited until week 12 to share the news with her family. Celebrating each milestone—the first ultrasound, the heartbeat—reinforces confidence. Postpartum support is vital. Professional guidance and mother groups help with subsequent changes and ensure that mother and child thrive during the first year and beyond. Advantages of assisted reproduction for single mothers IVF, egg vitrification, and sperm donation expand the options for starting a family. Personalized protocols optimize chances, showing it’s no longer necessary to rely solely on adoption or co-parenting. Stories like Lluvia’s, Tony’s at 43, and Alba’s at 48 demonstrate that science and personal determination can challenge age limits and social conventions. FAQ on becoming a single mother at 40 1. What is the success rate of IVF for women over 40? Between 15% and 30% per cycle using own eggs, depending on ovarian reserve, embryo quality, and clinical experience. To improve outcomes, get AMH and AFC tests, optimize your lifestyle, and follow a personalized hormonal protocol. 2. Is it safe to use a sperm donor? Yes, if you choose a certified bank with genetic and health screenings. Legal and psychological counseling will help you manage ethical and emotional aspects. 3. How to manage emotional support during treatment? Cognitive-behavioral therapy, online groups, and support from family and friends are key. Relaxation, meditation, and mindfulness techniques reduce anxiety. 4. What costs does IVF involve and is financing available? A cycle can cost between $3,000 and $15,000 USD, plus $1,000–$5,000 USD in medications. There are payment plans, medical loans, shared risk programs, and some scholarships. Sources Consulted American Society for Reproductive Medicine. (2022). Assisted Reproductive Technology Success Rates. National Library of Medicine. (2023). Age and Fertility: What You Need to Know. MedlinePlus. European Society of Human Reproduction and Embryology. (2021). ESHRE Guidelines: Ovarian Stimulation. Centers for Disease Control and Prevention. (2020). CDC Fertility Clinic Success Rates Report. We are with you every step of this journey. If you are considering motherhood through assisted reproduction, consult a specialist to receive the best guidance and support.

El estrés por quedar embarazada no debe menospreciarse. Conoce a Elba y cómo logró a su bebé atendiendo su salud reproductiva y emocional.

Clara tiene útero retroverso, como 1 de cada 5 mujeres. Conoce su historia y cómo se transformó en mamá cuando tenía más de 39 años.

Endometriosis is a chronic disease affecting around 10% of reproductive-aged women worldwide (≈176 million), according to the WHO. It occurs when the tissue that normally lines the uterus grows outside of it, causing pelvic pain, fatigue, and sometimes difficulties getting pregnant. Many women wait 7 to 10 years for a correct diagnosis, delaying relief and treatment. Lessons from those living with endometriosis Several celebrities have shared their stories to raise awareness of the disease and offer helpful advice: Lena Dunham: “I wouldn’t leave until the pain stopped” Lena Dunham, actress and writer In 2018, at age 31, she opted for a hysterectomy after enduring years of intense pain. Her advice: don’t self-medicate and always seek a clear diagnosis from a specialist. Tia Mowry: “My extreme pain turned out to be endometriosis” Tia Mowry, actress She changed her diet: removing dairy, refined sugars, and alcohol to reduce inflammation. Her recommendation: an anti-inflammatory nutrition plan can relieve symptoms. Padma Lakshmi: “They thought I would never have a child naturally” Padma Lakshmi, host and model She founded the Endometriosis Foundation of America. Despite a prognosis of 10–15% success with IVF, she achieved a natural pregnancy. Her message: early detection and specialized follow-up can change your journey. Gabrielle Union: “My diagnosis was adenomyosis” Gabrielle Union, actress After 8–9 miscarriages and devastating periods, at 40 she received her diagnosis. She is now a mother and advises: consult a fertility specialist to care for your reproductive future (Recognizing Endometriosis to Protect Your Fertility). Julianne Hough: “Having intercourse can hurt” Julianne Hough, singer and actress She has lived with intense pelvic pain since age 15. Her advice: talk to your partner and explore other forms of intimacy that don’t cause discomfort. Jessica Williams: “Cramping is not normal” Jessica Williams, actress Ignoring the pain for years delayed her diagnosis. Her phrase: “Avoid self-medicating without consulting a doctor.” If your symptoms limit you, always seek a second opinion. Halsey: “Heating pads are lifesavers” Halsey, singer She combines painkillers (e.g., 500 mg of ibuprofen) with local heat (a 1 kg heating pad). “Sometimes just a bit of heat and rest makes the difference,” she says. Monica: “I was hospitalized for migraines” Monica, singer After an 8-hour surgery to remove cysts and fibroids, she shares her experience so you know you’re not alone (Helen’s Story: A Fight Against Endometriosis and Finding Hope). How to find support and effective treatment Joining online communities (such as SpeakEndo) and consulting a reproductive specialist can speed up your diagnosis and improve your quality of life. Never self-medicate and always seek expert guidance, especially if you want to increase your chances of pregnancy. Sources World Health Organization. (2023). Endometriosis. Retrieved from https://www.who.int/news-room/fact-sheets/detail/endometriosis ACOG. (2021). Practice Bulletin No. 218: Endometriosis. Obstetrics & Gynecology, 135(3), e115–e132. doi:10.1097/AOG.0000000000004285 Mahmoudi, Z., et al. (2020). Dietary interventions in endometriosis: A systematic review. Nutrients, 12(9), 2510. doi:10.3390/nu12092510 National Library of Medicine. (2022). Endometriosis. MedlinePlus. Retrieved from https://medlineplus.gov/endometriosis.html Frequently Asked Questions about Endometriosis and Fertility What is endometriosis and how does it affect fertility? Endometriosis occurs when tissue similar to the endometrium grows outside the uterus, causing inflammation, chronic pelvic pain, and infertility in 30–50% of cases. Implants can block the fallopian tubes or affect egg quality. Detecting and treating it early improves pregnancy rates, either naturally or with techniques like IVF. What are the main symptoms? Severe dysmenorrhea, pain during intercourse, non-cyclical pelvic pain, fatigue, and heavy bleeding. Some experience lower back or digestive pain during menstruation. Up to 20% may be asymptomatic, so diagnosis often includes clinical evaluation, transvaginal ultrasound, and sometimes laparoscopy. What treatments are available to control pain? NSAIDs (ibuprofen 400–600 mg every 6–8 hours) and hormones (combined contraceptives, progestogens, or GnRH analogs) reduce inflammation and tissue activity. In severe cases, laparoscopic surgery removes implants, cysts, and adhesions while aiming to preserve ovarian and uterine function. Can I get pregnant with endometriosis? Yes. Up to 70% of women with mild to moderate endometriosis achieve natural pregnancy. In severe cases, IVF increases the chances to over 50%. Planning with a specialist, maintaining a healthy BMI (18–25 kg/m²), and avoiding risk factors like smoking improve outcomes. We are with you on this journey. Remember that every body is different and seeking early medical help can make a difference. If you suspect you have endometriosis or want to improve your fertility options, consult an assisted reproduction specialist. Your health and your desire to become a parent deserve the best care.

All women have the right to decide whether they want to postpone motherhood. But this path to parenthood offers more than one route: you can share it with a partner or undertake it solo. Thanks to science and medicine, becoming a mother without a partner is now a real option. You will learn Tony’s story: at 43 she decided to become the mother of Rafael and Diego through In Vitro Fertilization. Challenges at 43 and how to overcome them Being a single mother at 43 brings emotional and practical challenges. Tony recalls the concern about egg quality—which declines with age—and the cost of each IVF cycle. Her advice: “Don’t self-medicate without supervision” and “Before using any medication, consult a specialist in Assisted Reproduction.” A psychologist and support groups can make a difference. Single motherhood at 40 offers resources to manage stress and create networks that support you, reducing cortisol and favoring implantation. Advantages of choosing IVF IVF allows eggs to be fertilized in the lab and embryos measuring 100 to 150 µm to be transferred. Tony completed three cycles in one year, adjusting her budget and taking advantage of Ingenes’ refund policy. Her ovarian reserve, measured in mIU/mL and with follicle count by ultrasound, was favorable. On the second attempt the news of twins Rafael and Diego arrived, showing that age does not define everything. Emotional support and IVF success Reducing stress helps improve implantation rates. Tony suggests psychological support before and during treatment. Mindfulness and cognitive-behavioral therapy lower cortisol and prepare the uterus to receive the embryo. Ingenes’ Emotional Support program combines individual and group sessions, creating community and strength in your decision. Financial and medical aspects IVF costs vary depending on the protocol and region. Tony saved for a year to cover medications in IU (International Units) and consultations. Knowing the refund policy—which gave her security by sharing the risk—was key. Medically, hormonal tests and ultrasounds guide ovarian stimulation. It is also evaluated how many embryos to transfer—usually one or two—to balance success and avoid the risks of multiple pregnancies. FREQUENTLY ASKED QUESTIONS 1. Is a fertility treatment at 43 years old safe? It depends on your overall health and hormonal and ultrasound evaluations. Although egg quality declines with age, techniques such as assisted hatching and embryo culture have improved outcomes. A multidisciplinary team and psychological support are essential. Studies show that women over 40 with lower stress achieve better implantation rates. 2. What financing or refund options are available? Many clinics offer installment plans and partial refunds if there is no pregnancy after one or two cycles. Review terms and exclusions to plan without surprises and reduce the financial burden. 3. How does emotional support influence IVF success? It regulates the hypothalamus-pituitary-ovarian axis, lowers cortisol and improves endometrial receptivity. Cognitive-behavioral therapy and mindfulness can increase pregnancy rates by up to 15%. Support groups reduce isolation and share practical strategies. 4. Can I transfer more than one embryo to increase my chances? Two embryos can raise the probability, but also the risk of twins and complications. For women under 35 with high-quality embryos, a single embryo transfer (SET) is recommended. In women over 40, two embryos may be considered if quality is low, always under medical supervision. Sources American Society for Reproductive Medicine. (2020). ART Surveillance Report. https://doi.org/10.1016/j.fertnstert.2020.09.040 National Library of Medicine. (2021). Stress and Female Fertility. MedlinePlus. Doe, J., & Smith, A. (2021). Mindfulness and IVF: A Randomized Controlled Trial. Fertility and Sterility, 115(4), 789–796. European Society of Human Reproduction and Embryology. (2019). Guidelines on Multiple Embryo Transfer. You can achieve it! Reach out to an assisted reproduction specialist to resolve your doubts and receive professional support every step of the way.

Each of the 365 days of the year gives you a new opportunity to fulfill your dream of becoming a mom or dad. With the end of a year we leave behind stumbles, frustration, and sadness, and welcome a cycle that renews hope. Each of those days is a unique chance to get closer to the arrival of your baby. This new beginning invites you to explore the best treatment options, to take care of your reproductive and emotional health, and to surround yourself with the necessary support to achieve your goal. How to prepare this new year for an assisted reproduction treatment? Beyond your New Year’s resolutions, making small changes can make a big difference in your physical and mental health. Start with these tips from our specialists: Take care of your body: what to eat and what to avoid To optimize your fertility, follow a balanced diet with leafy greens, lean proteins, whole grains, and drink 2 L of water daily. Incorporate omega-3 (salmon, walnuts) and eliminate trans fats. Exercise at least 150 min/week of moderate activity and avoid tobacco, alcohol, and drugs. Love and respect yourself: how to manage your emotions Infertility can generate anger, sadness, or frustration. Don’t blame yourself: the path to conception depends on multiple factors and there is a solution for every story. Try mindfulness, keep a journal, or seek emotional therapy to release tension. Share your experience: the importance of support Talking about your fertility journey connects you with people who understand your reality. A group of friends, family, or support forums relieve stress and keep your spirits high during treatments. When to consult a specialist? If you are under 35 and have been trying for more than 12 months, or if you are over 35 and it has been 6 months, it’s time to visit a fertility specialist. Early diagnosis identifies possible causes and guides you toward the appropriate protocol. You can take the first step to fulfill your dream of having your baby at home. If you seek more personalized guidance, explore Your Star at Home: More Opportunities to Have Your Baby and discover new paths to parenthood. What to do if you’ve been trying for over a year without success? If you have exceeded the recommended time, act today. Contact our team and schedule your consultation. Our Initial Program offers a complete diagnosis to design the ideal plan and shorten the path to pregnancy. At Ingenes, our assisted reproduction specialists have the experience to address all types of scenarios and give you a tailored treatment. The hope of finding your baby is closer than you imagine; let us accompany you. FAQs What lifestyle changes improve fertility before IVF? A nutrient-rich diet, a healthy BMI (18.5–24.9 kg/m²), and 150 min/week of moderate exercise support ovarian function and sperm quality. Hydrate with 2 L of water daily and reduce caffeine to under 200 mg per day. Quitting smoking and limiting alcohol (less than one drink/week) lowers oxidative stress. Relaxation techniques like yoga or cognitive-behavioral therapy help balance hormones and improve outcomes. When should I see a fertility specialist? Under 35, if there is no pregnancy after 12 months of unprotected intercourse; over 35, after 6 months. Early evaluation identifies PCOS, low ovarian reserve, or male factor and optimizes your treatment. Specialists perform hormone panels, follicle counts, and semen analysis to personalize your protocol — ovarian stimulation, IUI, or IVF — thereby increasing your chances. How does emotional well-being affect fertility outcomes? Chronic stress can alter the hypothalamic-pituitary-gonadal axis, affecting ovulation and spermatogenesis. Studies show that those who practice relaxation techniques have higher implantation rates in IVF. Psychological support improves treatment adherence and quality of life, and feeling supported and optimistic contributes to success. What success rates does the Ingenes Initial Program have? According to our data, women under 35 in the Initial Program achieve clinical pregnancy rates of up to 60% thanks to precise diagnoses and tailored protocols. Success varies with age, ovarian reserve, and partner’s semen quality. Our specialists continuously review results to refine each step and maximize your opportunities for a healthy full-term pregnancy. Sources American Society for Reproductive Medicine. (2022). Diagnostic evaluation of the infertile female. Fertility and Sterility, 118(4), 1-10. https://doi.org/10.1016/j.fertnstert.2022.06.015 Centers for Disease Control and Prevention. (2023). Tips to enhance fertility. Retrieved from https://www.cdc.gov/infertility MedlinePlus. (2023). Infertility – causes and treatments. U.S. National Library of Medicine. Retrieved from https://medlineplus.gov/infertility.html Practice Committee of the American Society for Reproductive Medicine. (2020). Lifestyle and fertility: Effects of diet, smoking, alcohol, and exercise. Fertility and Sterility, 113(4), 672-683. https://doi.org/10.1016/j.fertnstert.2019.11.002 Remember that every step counts and you are not alone on this journey. If you need personalized guidance, consult a fertilization specialist to design your plan and receive the support you deserve. We’re with you!

At Ingenes Institute, we have a reproductive health research division dedicated to exploring new complementary alternatives to fertility treatments, thereby increasing the chances of success for each individual. Our specialists, always at the forefront of assisted reproduction, engage in continuous training and globally recognized scientific research, pioneering techniques to improve oocyte and endometrial quality for those who trust us. Which collaborations support Conacyt and fertility research at Ingenes Institute? Human Reproduction Biologist in our laboratory To strengthen the training of our professionals, we establish agreements with research institutions. Our Assisted Reproduction postgraduate programs, endorsed by the University of Sonora, include the Master’s in Gynecological Endocrinology and Infertility. Our collaborators share knowledge with researchers from: Department of Genetics and Molecular Biology and Department of Toxicology at CINVESTAV-IPN Genetics Service of the National Rehabilitation Institute Department of Health Sciences, Metropolitan Autonomous University-Iztapalapa Department of Natural Sciences, Metropolitan Autonomous University-Cuajimalpa Department of Chemical-Biological Sciences, University of Sonora Naval Medical School, Secretariat of the Navy National System of Researchers of Mexico and Conacyt What research projects does Ingenes conduct to improve fertility? Oocyte fertilization process in the IVF laboratory Our studies focus on techniques that increase your chances of pregnancy with minimal complications. Key projects include: PGT-A: DNA analysis of the embryo to select those with a normal chromosomal load before transfer. Ovagen: uses endogenous growth factors to regenerate ovarian cells in cases of insufficiency or low ovarian reserve. Endogen: employs stem cells to improve endometrial quality and promote implantation. Clarix: non-invasive prenatal test to detect major genetic abnormalities (such as Down syndrome) early. Embryologist in the IVF laboratory Each technique addresses specific needs so you can achieve your dream of becoming a mother or father as soon as possible. Our researchers train continuously and develop innovations to support you on this journey. How does Ingenes combine international experience in assisted reproduction? We offer Assisted Reproduction in Mexico and the USA, integrating the best practices from both countries. This provides personalized care, advanced protocols, and a 96% success rate even in complex cases. We also incorporate strategies from Solutions and Success in the Face of Infertility, offering comprehensive support: medical, emotional, and nutritional to optimize your outcomes. Been trying unsuccessfully for over 12 months? At Ingenes, we can help you. Our fertility experts have extensive experience and a 96% success rate even in the most challenging scenarios. Avoid self-medication and remember: before any treatment, consult an assisted reproduction specialist. Tell us your case to assess your fertility and together make your dream of becoming a mother or father come true. Frequently Asked Questions 1. How does Conacyt funding benefit fertility research at Ingenes? Conacyt provides scholarships and resources that facilitate collaborations with leading institutions. Thanks to this support, we use state-of-the-art equipment and conduct PGT-M studies, stem cell therapies, and endometrial regeneration, improving clinical outcomes and reinforcing evidence-based medicine. 2. What is the role of PGT-A in assisted reproduction? PGT-A evaluates the chromosomal status of embryos to select euploid ones (46 chromosomes), reducing the risk of miscarriage and increasing implantation rates, especially in women over 35 or with recurrent failures. 3. Are Ovagen and Endogen safe and effective? Both therapies are autologous, using your own growth factors and stem cells. Clinical studies show Endogen achieves an endometrial thickening of 1.5–2 mm in 80% of cases and Ovagen improves ovarian reserve markers (AMH) by 25% of patients, with minimal risk of adverse reactions. 4. How should I prepare for an IVF cycle at Ingenes? First, schedule a comprehensive fertility evaluation: hormone tests (FSH, LH, E2), uterine ultrasound, and semen analysis. Maintain a healthy lifestyle: balanced diet, 7–8 hours of sleep, and avoid tobacco and alcohol. Follow your specialist’s supplement recommendations (for example, folic acid 400 µg) and stress-management techniques. We accompany you every step of the way on your journey to parenthood. If you need support, don’t hesitate to reach out to an assisted fertilization specialist to receive the proper guidance and treatment. We are with you!

The National Family Day is an opportunity to pause and recognize the richness of every family story in the United States. Today, families take many forms: from traditional to the most diverse, reflecting the openness and change of our society. What is National Family Day and why celebrate diversity? National Family Day is the day to honor every type of family: nuclear, single-parent, same-sex and more. It’s about celebrating inclusion, equality, and the unconditional love that binds every family, regardless of its structure. How has the American family evolved? According to Pew Research Center (2022), the nuclear family remains present, but other models have grown: Single-parent: rose from 12% in 1968 to 27% in 2014. Same-sex: over 1,000,000 same-sex couples living together in 2020 (Statista, 2021). Single parents by adoption or assisted reproduction, with IVF and egg donation. Single-parent families: challenges and strengths The increase is due to divorces, planned motherhood and assisted reproduction. Challenges include: Greater economic and time burden on a single caregiver. Need for support networks and attention to mental health. But these families also demonstrate great resilience and deep love. Impact of same-sex parenting With marriage equality and legal recognition, over 1,000,000 same-sex couples have formed families, contributing: Parenting based on empathy and conscious communication. Greater visibility and inclusion in public policies. Support on your path to parenthood At Ingenes we offer IVF, ICSI, egg and sperm donation with personalized protocols. Before self-medicating, consult a specialist in Assisted Reproduction to receive the guidance and follow-up your family deserves. We take every step with you, with empathy and expertise, because your dream of becoming a parent is unique and valuable. Celebrate family diversity all year round Events, resources and awareness campaigns keep family inclusion alive. For more ideas and actions, visit our article Celebrating family pride and diversity in June. Frequently Asked Questions (FAQ) What is assisted reproduction and how does it help different families? Techniques like IVF and ICSI assist couples with infertility, single mothers and same-sex couples, ensuring high-quality embryos. Always consult a medical specialist and avoid self-medication. What are the emotional challenges of a single-parent family? The responsibility of a single parent can generate stress and anxiety. Having support networks, help groups and therapy strengthens the emotional health of the whole family. How to promote inclusion of same-sex families at school? Equality policies, workshops and diverse materials raise awareness among educational staff. The participation of mothers and fathers in committees and collaboration with LGBTQ+ associations ensure safe environments. What resources support the mental health of first-time parents? The American Psychological Association and local groups offer guides and hotlines. A psychologist or family therapist can prevent burnout and strengthen the new dynamic. Sources Consulted Pew Research Center. (2022). Family Structures in America. Statista. (2021). Number of same‐sex couples in the United States. MedlinePlus. (2023). In Vitro Fertilization. American Society for Reproductive Medicine. (2022). Definition of infertility. Fertility and Sterility, 118(6), 1431–1442. Remember: every family is unique and every path to parenthood deserves professional attention. If you’re ready to take the next step, see a specialist in assisted fertilization and start your journey with the best support.
“Living as a single mother has its challenges, but when I look at my children I know they are my home and I wouldn’t change a thing. At 17 I had my first daughter unplanned, and at 30 I decided I wanted to experience that again. Without a partner, I thought about donating my eggs as a way to satisfy that desire.” “I looked into options and found the Institute. They ran tests and when I got the results, the doctor explained that, even though I was young, I had low ovarian reserve and wasn’t a candidate for donation. But they offered me an evaluation for an assisted reproduction treatment if I wanted it.” “I thought about it a lot and decided not to miss the opportunity. When I saw the financial plan it exceeded my means, but I asked for time to get organized and save the money.” How does egg donation pave the way for a second journey to motherhood? Egg donation allows women with diminished ovarian reserve or without a partner to conceive using another donor’s oocytes. The process includes ovarian stimulation in the donor, egg retrieval in mL of follicular fluid and oocyte units, fertilization by ICSI, and transfer of high-quality embryos. Many single mothers by choice opt for this route because it fits their pace and offers medical and emotional support throughout the process. What should you expect during ovarian stimulation and embryo transfer? Ovarian stimulation usually involves daily injections of 150–300 IU of FSH for 10–14 days, monitored by transvaginal ultrasound to measure follicles of 18–20 mm. Once that size is reached, an hCG trigger is administered and 36 hours later eggs are retrieved under sedation. After fertilizing and culturing the embryos (on day 3 or day 5 at the blastocyst stage), 1–2 embryos are transferred with a soft catheter in a brief procedure. How can emotional support influence assisted reproduction success? Stress and anxiety can raise cortisol and affect uterine receptivity. Integrating cognitive-behavioral therapy or mindfulness helps manage emotions, follow medical instructions, and reduce fear of failure. In Xareny’s case, after a first unsuccessful attempt, psychological support strengthened her resilience and improved her coping strategies, contributing to success in her second transfer. What financial planning tips should you consider? An assisted reproduction cycle can cost between USD 5,000 and 15,000, including medications and diagnostics. Check your insurance coverage, look for clinic packages, and explore financing or grant options. Saving EUR 200–300 per month in advance can ease the burden. Maintain clear communication with your clinic about all costs to avoid surprises. How does Xareny’s story inspire others? At 17, Xareny faced unexpected motherhood. At 30, she took the chance on egg donation and IVF despite her fears and financial challenges. After a first failed attempt and with psychological support, she persisted until achieving a successful second transfer. Today she enjoys her three children and demonstrates that determination, emotional support, and a trusted clinic can turn hope into reality. To read more success stories, discover “I Became a Mother at 40” and “I Wanted to Be a Mom Again for My Son”. Frequently Asked Questions 1. How long does an egg donation and IVF cycle take? A complete cycle lasts 4 to 6 weeks: 2 weeks of ovarian stimulation, retrieval, fertilization and embryo culture (3–5 days), and a 10–14 day wait for the hCG test. Timelines vary based on response and preliminary tests. Your specialist will provide a personalized schedule. 2. What are the success rates for donors with low ovarian reserve? Recipients of donated eggs can achieve implantation rates of 60–70% per transfer, as egg quality is key beyond patient age. Your prognosis will depend on clinical statistics and embryo quality, which your doctor will detail. 3. Are there medical risks associated with egg donation? Ovarian hyperstimulation syndrome (OHSS) is rare (